 Most people are familiar with the term Chronic Obstructive Pulmonary Disease (COPD). You may have watched commercials explaining its symptoms or have seen digital ads demonstrating how patients can treat COPD and other impaired breathing conditions, such as asthma and chronic bronchitis.
Most people are familiar with the term Chronic Obstructive Pulmonary Disease (COPD). You may have watched commercials explaining its symptoms or have seen digital ads demonstrating how patients can treat COPD and other impaired breathing conditions, such as asthma and chronic bronchitis.
Have you ever wondered why you know so much about COPD, yet you rarely hear the term bronchiectasis?
COPD vs. Bronchiectasis:
 COPD is a highly researched and investigated chronic lung disease that affects more than 11 million people within the United States. The term is used by medical professionals to describe a range of pulmonary conditions that cause shortness of breath, inflammation in the airways, or impair an individual’s ability to breathe. Patients who are diagnosed with COPD may experience frequent pneumonias, airway irritation, and permanent damage to the lungs. According to the American Lung Association, COPD is considered the third leading cause of death in America.1
COPD is a highly researched and investigated chronic lung disease that affects more than 11 million people within the United States. The term is used by medical professionals to describe a range of pulmonary conditions that cause shortness of breath, inflammation in the airways, or impair an individual’s ability to breathe. Patients who are diagnosed with COPD may experience frequent pneumonias, airway irritation, and permanent damage to the lungs. According to the American Lung Association, COPD is considered the third leading cause of death in America.1
Because of its prevalence in respiratory medicine, COPD has become a household name. But did you know it’s estimated that bronchiectasis affects more than 4.2 million people in America?2

What We Know About Bronchiectasis:
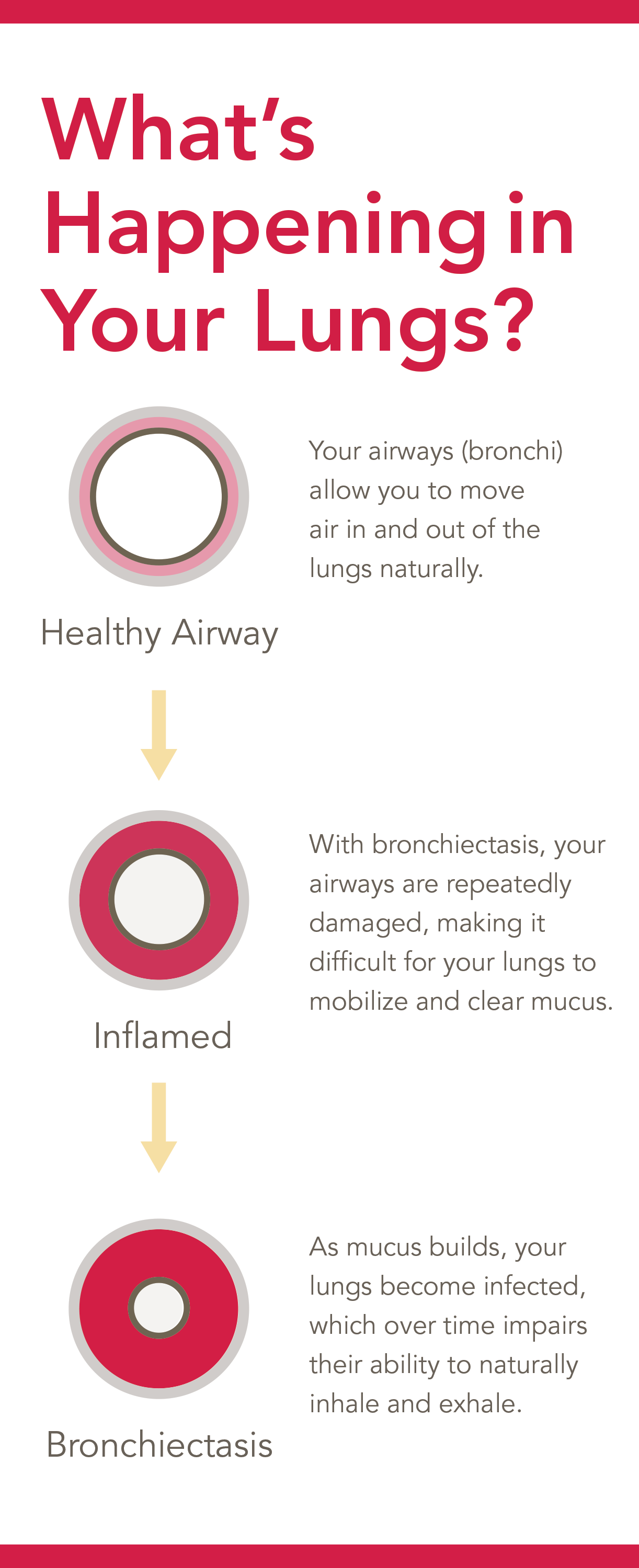
Bronchiectasis (brong-kee-EK-tuh-sis) is an irreversible lung disease that permanently damages a person’s airways through a recurring cycle of inflammation and infection in the lungs. As airways are repeatedly damaged, patients are unable to mobilize and clear mucus—allowing bacteria to infect the lungs, which over time weakens their ability to move air in and out.
Bronchiectasis is commonly caused by repeated exacerbations, whereas COPD generally results from smoking, allergies, or pollution. However, it is possible for someone to have COPD and bronchiectasis, and experience bronchiectasis-related symptoms. In fact, a peer-reviewed study was conducted to examine the occurrence of non-cystic fibrosis bronchiectasis among U.S. adults in 2013.3 The research suggests that approximately 52% of COPD patients also reported bronchiectasis-related symptoms and that the chronic pulmonary condition was more prevalent in women than in men.
 Although additional research is needed to enhance the study of effective bronchiectasis treatment, the findings of a 2018 longitudinal outcome-based study demonstrate the efficiency of high frequency chest wall oscillation therapy (HFCWO), via the SmartVest Airway Clearance System, in decreasing hospitalizations (42%) and reducing antibiotic therapy (38%).4
Although additional research is needed to enhance the study of effective bronchiectasis treatment, the findings of a 2018 longitudinal outcome-based study demonstrate the efficiency of high frequency chest wall oscillation therapy (HFCWO), via the SmartVest Airway Clearance System, in decreasing hospitalizations (42%) and reducing antibiotic therapy (38%).4
HFCWO is an airway clearance technique in which a patient wears a respiratory vest that produces oscillations to loosen mucus from the airways, which is cleared from the lungs through a productive cough.
What We Don’t Know About Bronchiectasis:
In an article titled “Bronchiectasis: An Emerging Global Epidemic,” authors Sanjay H. Chotirmall and James D. Chalmers stress the urgency to prioritize bronchiectasis research-based analysis, worldwide, and encourage future collaboration among medical professionals on the study of bronchiectasis, in terms of its genetic heterogeneity and treatments.5
According to Chotirmall and Chalmers, bronchiectasis-related topics that require further exploration include:
- A deeper understanding of the direct causes of the condition,
- Additional research on how the lung disease can develop in patients, with focus on individual symptoms, and
- Further investigation on airway microbes in a patient’s lungs that are linked to bronchiectasis, including viruses and fungi.
Another critical area of study that requires further emphasis is addressing the overwhelming lack of bronchiectasis education that clinicians and patients can access. Such limited resources play a significant role in the absence of bronchiectasis awareness among the general public.
Fortunately, new research continues to be developed. At the third annual World Bronchiectasis Conference, new clinical evidence was presented evaluating bronchiectasis-related exacerbations using HFCWO therapy.6 The study reported non-cystic fibrosis bronchiectasis patients experienced a significant reduction in the number of severe exacerbations requiring hospitalization after using SmartVest.
Why Is Bronchiectasis Underdiagnosed?
Electromed’s recent video series, titled “Ask a Pulmonologist,” features Dr. Frederic Seifer, a renowned pulmonologist who has helped expand the study of bronchiectasis and how to treat its symptoms. In the first episode of the series, “Why is Bronchiectasis Overlooked?,” Dr. Seifer explains that while in medical school, physicians receive limited education on bronchiectasis. Therefore, without a comprehensive knowledge or even familiarity with the condition on how to accurately diagnosis or treat its symptoms, it becomes even more difficult to recognize bronchiectasis as an individual condition. Instead, clinicians may categorize it under the umbrella of COPD.
Why Further Research Is Needed to Expand Bronchiectasis Awareness

Understanding bronchiectasis is the first step to spreading awareness among clinicians and helping them find the best defense for their patients’ chronic symptoms. Although additional research is necessary to advance this area of respiratory medicine, there have been significant strides made by medical professionals to further our understanding of bronchiectasis. For example, the World Bronchiectasis Conference hosts leading experts on bronchiectasis and nontuberculous mycobacteria to discuss recent clinical findings. The conference has had a profound impact on this lesser known chronic lung condition, as each year, experts share recent clinical data that inspires further exploration—all with the end goal of helping patients manage their symptoms without compromising their quality of life.
How Can You Help Spread the Word About Bronchiectasis?
To learn more about bronchiectasis, visit SmartVest.com and discover a wealth of patient resources, including clinical studies on how HFCWO therapy helps patients manage their symptoms.
-
American Lung Association (n.d.) How serious is COPD. Retrieved from https://www.lung.org/lung-health-and-diseases/lung-disease-lookup/copd/learn-about-copd/how-serious-is-copd.html
-
Weycker, D. Hansen, G. Seifer, F. (2017). Prevalence and incidence of noncystic fibrosis bronchiectasis among US adults in 2013. Chronic Respiratory Disease, 14(4). 377-384. doi 10.1177/1479972317709649.
-
Weycker, D. Hansen, G. Seifer, F. (2017). Prevalence and incidence of noncystic fibrosis bronchiectasis among US adults in 2013. Chronic Respiratory Disease, 14(4). 377-384. doi 10.1177/1479972317709649.
-
Sievert, C. Beaner C. (2018). Incidence of bronchiectasis-related exacerbation rates after high frequency chest wall oscillation (HFCWO) treatment: A longitudinal outcome-based study. Respiratory Therapy, 13(2). Retrieved from https://smartvest.com/clinical-evidence/incidence-bronchiectasis-related-exacerbation-rates-after-hfcwo-treatment-longitudinal-outcome-based-study/
-
Chotirmall, S. and Chalmers, J. (2018). Bronchiectasis: An emerging global epidemic. Medscape, 18(76). Retrieved from https://www.medscape.com/viewarticle/897818_print
-
SmartVest (2018). New evidence demonstrates SmartVest may help reduce hospitalizations and stabilize lung function. Retreived from https://smartvest.com/new-evidence-demonstrates-smartvest-benefits/

