
Chronic lung diseases like bronchiectasis and cystic fibrosis cause irreversible damage to the lungs and airways, making it difficult to breathe and break up mucus buildup.
Other respiratory conditions, like asthma, force the airways to narrow due to swelling (i.e., inflammation), causing the muscles around the airways to tighten. As a result, breathing feels more labored.
Although each person will experience symptoms differently, many lung conditions share similarities, particularly shortness of breath, wheezing, and excess mucus production—all of which can worsen over time and disrupt our ability to breathe independently.
However, each condition varies in how it can cause a person to develop breathing difficulty.
How Do Restrictive vs. Obstructive Lung Disease Differ?
 Chronic lung conditions typically fall into two categories: restrictive vs. obstructive. The primary difference between the two is that obstructive diseases are caused by blockages in the airways that obstruct your ability to expel air. In contrast, restrictive conditions affect the size or capacity of the lungs to take in air (i.e., the volume of air it can hold).¹
Chronic lung conditions typically fall into two categories: restrictive vs. obstructive. The primary difference between the two is that obstructive diseases are caused by blockages in the airways that obstruct your ability to expel air. In contrast, restrictive conditions affect the size or capacity of the lungs to take in air (i.e., the volume of air it can hold).¹
To help you understand the difference between obstructive and restrictive lung conditions, this guide will provide the following insights:
- Outline the underlying causes and symptoms of each condition
- Identify which conditions fall into each category
- Discuss treatment options that may help you find symptom relief
Understanding Obstructive Lung Disease
Obstructive lung diseases are categorized as conditions that restrict airflow from your lungs. For example, think about each time you exhale. When your airways become inflamed and narrowed—due to smoke, airborne irritants, allergies, etc.—you cannot empty your lungs completely.
As a result, breathing may feel more labored and is often accompanied by wheezing.²
Examples of conditions that fall under the category of obstructive lung disease include COPD (chronic “obstructive” pulmonary disease) and asthma.
Symptoms generally include shortness of breath, wheezing, and coughing. People with this condition may also experience increased mucus production and chest tightness.
What Happens When Air Gets Trapped in Your Lungs?
Emphysema falls under the umbrella of COPD. It develops from repeated damage to the alveoli—the tiny air sacs of your lungs. When alveoli is healthy, your body can exchange oxygen and carbon dioxide as you inhale and exhale air.
falls under the umbrella of COPD. It develops from repeated damage to the alveoli—the tiny air sacs of your lungs. When alveoli is healthy, your body can exchange oxygen and carbon dioxide as you inhale and exhale air.
For example, as you inhale, the air sacs expand and transport oxygen to the bloodstream. In contrast, when you exhale, the air sacs shrink back down, forcing carbon dioxide out.
When blockage or obstruction occurs (due to inflammation), old air gets trapped inside the lungs. And over time, air sacs become overinflated and eventually rupture to form one larger air pocket.³
As a result, you may experience shortness of breath, cough, rapid breathing, and mucus production.4
Restrictive Lung Disease 101
Obstructive lung disease describes conditions that make exhaling air from the lungs difficult. Restrictive lung diseases affect a person’s ability to inhale air into the lungs. Your lungs cannot fully expand to take in oxygen with this condition.
Restrictive lung disease can be split into two categories: intrinsic lung restrictions and extrinsic lung restrictions.5
Intrinsic refers to issues happening inside a person’s lungs. For example, pulmonary fibrosis is a condition that occurs when lung tissue develops scarring.6
Over time, the scarred tissue becomes stiff, making it harder to expand the lungs as you inhale air. Unlike cystic fibrosis, pulmonary fibrosis is not a genetic condition that affects children. Instead, it typically develops in individuals over 50, especially those who smoke cigarettes or were regularly exposed to chemical substances.7
 Other examples of underlying conditions that affect the lungs’ ability to perform include:
Other examples of underlying conditions that affect the lungs’ ability to perform include:
- Interstitial lung disease
- Sarcoidosis
- Pneumoconiosis8
Extrinsic refers to conditions outside of the lungs that affect their ability to inhale properly. Obesity is an example of an extrinsic lung restriction because it puts pressure on the diaphragm, lungs, and chest wall. Again, this makes breathing challenging to perform.
Other conditions like scoliosis, a sideway curvature of a person’s spine, can restrict breathing due to chest distortion, which can cause the rib cage to press against the lungs.9
Certain neuromuscular diseases like muscular dystrophy can also weaken your lungs’ tissue over time, making it harder to breathe independently.10
Is Bronchiectasis Obstructive or Restrictive?
Now that you understand the differences between obstructive and restrictive lung diseases, you may wonder where bronchiectasis lands between these two categories.
Bronchiectasis is an irreversible lung condition that causes the airways to widen abnormally due to a repeated cycle of inflammation and infection. As the airways become damaged, the lungs slowly lose their ability to mobilize and clear mucus effectively. As a result, the cycle begins again, and the lungs experience more damage and buildup.
One of the most common symptoms of bronchiectasis is shortness of breath caused by inflammation and mucus buildup. Therefore, bronchiectasis makes it difficult to expel air from the lungs due to obstructed airways.
Bronchiectasis, COPD, asthma, and other chronic lung conditions fall under obstructive respiratory disease.
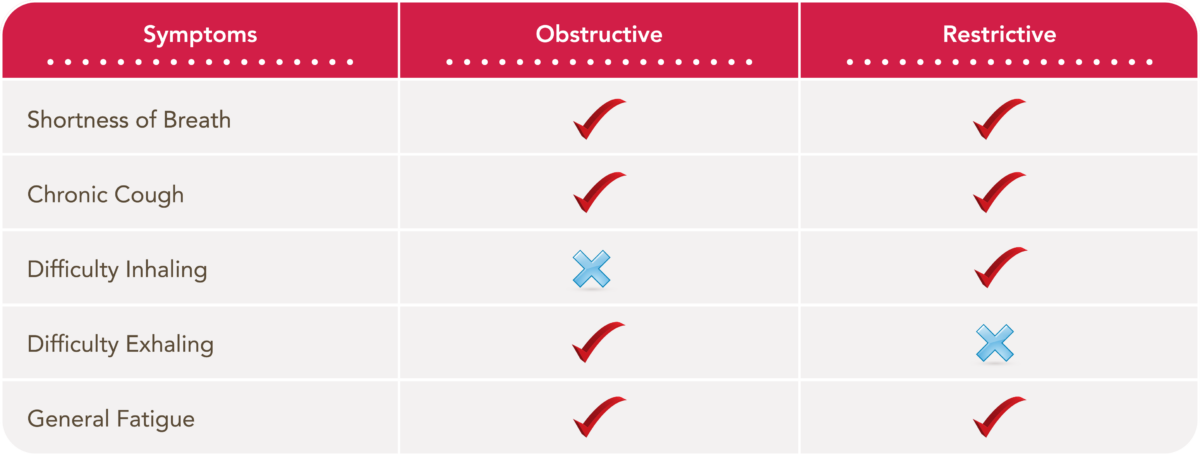
Diagnosing Obstructive and Restrictive Lung Diseases
Suppose you are experiencing any of the mentioned symptoms (i.e., shortness of breath, mucus buildup, wheezing, chronic cough, and repeated respiratory inflammation and infection). In that case, the next step is contacting your clinician for a diagnosis.
Your healthcare team may recommend a chest X-ray or high-resolution computerized tomography (HRCT) scan.
Note, an HRCT scan is the best way to receive an accurate bronchiectasis diagnosis. For more details, read our helpful guide on this advanced screening.
Depending on your individual symptoms, your clinician may also perform a spirometry test, which is a pulmonary function test that can measure how well (and how quickly) oxygen is entering and exhaling from your lungs.
The results of these tests can help provide a diagnosis and determine whether the condition affecting your lungs is obstructive or restrictive.
Treating Obstructive and Restrictive Lung Diseases
 Both obstructive and restrictive lung diseases require ongoing management. For example, managing obstructive lung conditions like COPD and bronchiectasis may involve medications such as bronchodilators and antibiotics to reduce inflammation or other symptoms, in addition to breathing exercises and airway clearance techniques.
Both obstructive and restrictive lung diseases require ongoing management. For example, managing obstructive lung conditions like COPD and bronchiectasis may involve medications such as bronchodilators and antibiotics to reduce inflammation or other symptoms, in addition to breathing exercises and airway clearance techniques.
Clinicians may prescribe oxygen or other respiratory support therapies to improve the patient’s breathing ability for restrictive lung diseases.
Coping with a Chronic Respiratory Illness
 Each person will experience airway obstruction or restriction differently. Clinical resources and local communities are available to help you find the support you need to improve your quality of life and ability to breathe independently.
Each person will experience airway obstruction or restriction differently. Clinical resources and local communities are available to help you find the support you need to improve your quality of life and ability to breathe independently.
If you’re living with an obstructive lung disease like bronchiectasis or COPD, now is the time to talk to your clinician about airway clearance via The SmartVest Airway Clearance System.
Using high-frequency chest wall oscillation (HFCWO) therapy, SmartVest delivers repeated air pulses that gently squeeze and release the upper chest wall to loosen and thin mucus, making it easier to propel mucus upward, so it’s easier to cough out.
The result is less blockage from mucus buildup and improved airway clearance to reduce the cycle of inflammation and infection.
If you’d like to learn more about how SmartVest can help you breathe easier and get back to living independently, request an information packet today and deliver it to your address.
Resources
- Johns Hopkins Medicine. “Restrictive Lung Disease.” Retrieved from https://www.hopkinsmedicine.org/health/conditions-and-diseases/restrictive-lung-disease
- Mayo Clinic. “Symptoms: Wheezing.” Retrieved from https://www.mayoclinic.org/symptoms/wheezing/basics/causes/sym-20050764
- Cleveland Clinic. “Emphysema.” Retrieved from https://my.clevelandclinic.org/health/diseases/9370-emphysema
- Johns Hopkins Medicine. “Pulmonary Emphysema.” Retrieved from https://www.hopkinsmedicine.org/health/conditions-and-diseases/pulmonary-emphysema
- Medical News Today. “How to Recognize and Treat Restrictive Lung Disease.” Retrieved from https://www.medicalnewstoday.com/articles/319012
- Mayo Clinic. “Pulmonary Fibrosis.” Retrieved from https://www.mayoclinic.org/diseases-conditions/pulmonary-fibrosis/symptoms-causes/syc-20353690
- Cleveland Clinic. “Pulmonary Fibrosis.” Retrieved from https://my.clevelandclinic.org/health/diseases/10959-pulmonary-fibrosis
- Medical News Today. “How to Recognize and Treat Restrictive Lung Disease.” Retrieved from https://www.medicalnewstoday.com/articles/319012
- Mayo Clinic. “Scoliosis: Symptoms and Causes.” Retrieved from https://www.mayoclinic.org/diseases-conditions/scoliosis/symptoms-causes/syc-20350716
- Medical News Today. “What Is Muscular Dystrophy?” Retrieved from https://www.medicalnewstoday.com/articles/187618

